ProMatrix Technology
Towards in vivo tissue engineering
ProMatrix - unlike ANY other Tissue Scaffold
A highly biological scaffold which, when grafted onto a wound bed, creates a new ‘tissue territory’ or 3D framework to guide and support tissue formation.
ProMatrix targets the early phase of wound healing and is designed to provide optimal properties to promote a regenerative type of tissue healing response.
The formation of new tissue naturally starts through the growth of progenitor cells around the wound. ProMatrix supports the migration of these progenitor cells into the scaffold framework, which are guided by the provisional structure to organise new tissue formation.
Application of ProMatrix BioDerm
ProMatrix BioDerm is for reconstructing deep or full-thickness skin loss wounds.
The wound bed must be surgically cleaned cleaned before applying the scaffold.
ProMatrix BioDerm is simply hydrated in surgical saline, or physiological solution, and gently transferred to the wound bed, and secured with sutures or surgical staples.
The wound is then covered with a semi-permeable layer such as perforated silicone membrane, and a moistened absorbent dressing. The dressings are changed twice weekly until regeneration is complete.
The use of ProMatrix to reconstruct skin after full-thickness skin loss.
Key properties of ProMatrix
Rapid vascularisation
Supports the rapid formation of blood capillaries within the structure from the patient’s own wound healing cells. Vascularisation integrates this new tissue territory with the body, and accelerates the process of tissue growth.
Rapid cellularisation
Supports the rapid ingrowth of fibroblast cells into the scaffold structure, together with the formation of new blood capillaries. The 3D scaffold structure organises the cells and provides space for these cells to replicate and build up a new tissue.
Rapid deposition of new Extra-cellular Matrix
Allows the cells within the scaffold to naturally deposit a permanent Extracellular Matrix, or network of collagen and other tissue proteins which forms the new tissue.
Scar-free outcome
The scaffold provides the structure which organises ingrowing cells to form new dermal tissue with a normal skin-like structure. This is in contrast to healing by secondary intention which results in build up of scar tissue.
How effective is ProMatrix technology?
The ultimate value of ProMatrix must lie in its effectiveness in supporting rapid cellular ingrowth, and in preventing scarring.
Current evidence on experimental evidence in vitro and in vivo. This is essential data to progress to clinical research, to gain definitive proof of effectiveness in people.
ANTI-SCARRING EFFECT In vitro
Scarring is the natural result of vigorous wound healing. Scar tissue looks different from normal tissue not just at the surface but also inside. It is caused by fibroblasts growing rapidly and piling up during the healing process, to form dense tracts of cells. These assemblies of fibroblasts both contract, and secrete collagen which form long thick fibres, manifest as scar contractures. Inside scar tissues, these features are hallmarks of fibrosis.
ProMatrix provides an alternative 3-dimensional space for fibroblasts to disperse through, instead of piling up as they multiply on top of one another. Additionally, the nano-scale fibre structure of the scaffold itself provides an intricate matrix for cells to adhere to.
These factors together result in a tissue scaffold which prevents scarring.
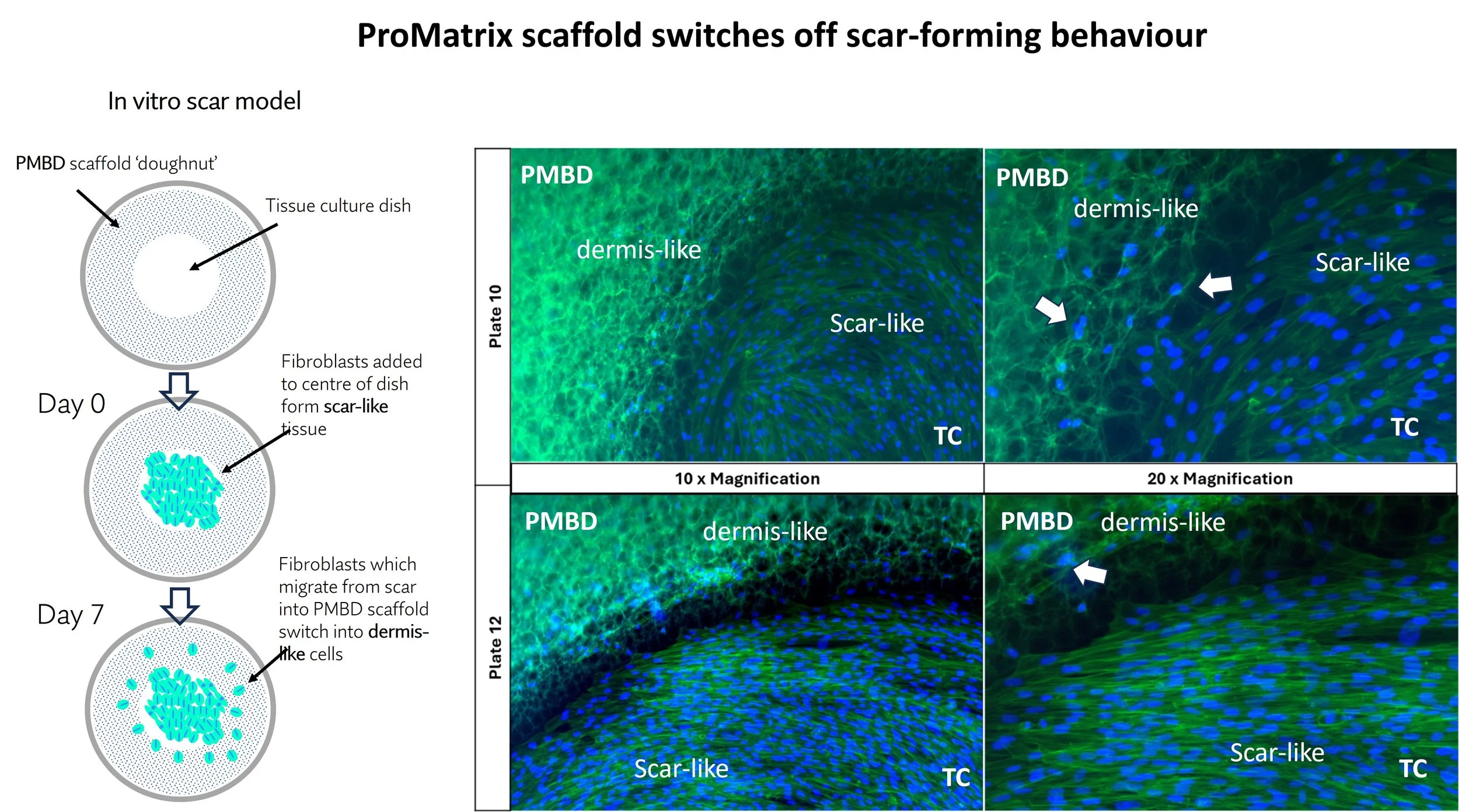
In this experimental model, human dermal fibroblasts are induced into a scar-like shape (morphology) and behaviour (phenotype). This is seen in the micrographs above, in the lower right side of each field-of-view.
The system comprises a ring of three-dimensional ProMatrix scaffold formed in a cell culture dish, surrounding the central zone of exposed culture surface. Fibroblasts are seeded into the central zone, and the entire dish is flooded with culture medium, and incubated at 37’C for several days. The experiment is terminated by chemical fixation, and cells are stained with green fluorescent reagent, (phalloidin-Alexa488), to identify the cytoskeleton (actin) proteins and counter-stained with blue fluorescent reagent (DAPI) to show cell nuclei.
The results show (i) the fibroblasts in the central zone rapidly grew, packed tightly together and formed characteristically elongated morphology, resembling scar tissue (bottom right of each micrograph). (ii) fibroblasts migrated from the ‘scar’ zone into the ProMatrix scaffold (upper left of each micrograph), and switched morphology from elongate and interconnected to rhomboid and solitary, resembling normal dermal tissue.
Significance
The migration of Human dermal fibroblasts from a scar-like phenotype into ProMatrix scaffold demonstrates an essential scaffold property.
ProMatrix structure acts as a template which guides the fibroblasts to adopt normal dermis mophology.
Scar-like behaviour can be switched to normal dermal behaviour can be achieved by cell-adhesive interactions with a tissue scaffold, without pharmacological agents.
Rapid integration and scarless reconstruction in vivo
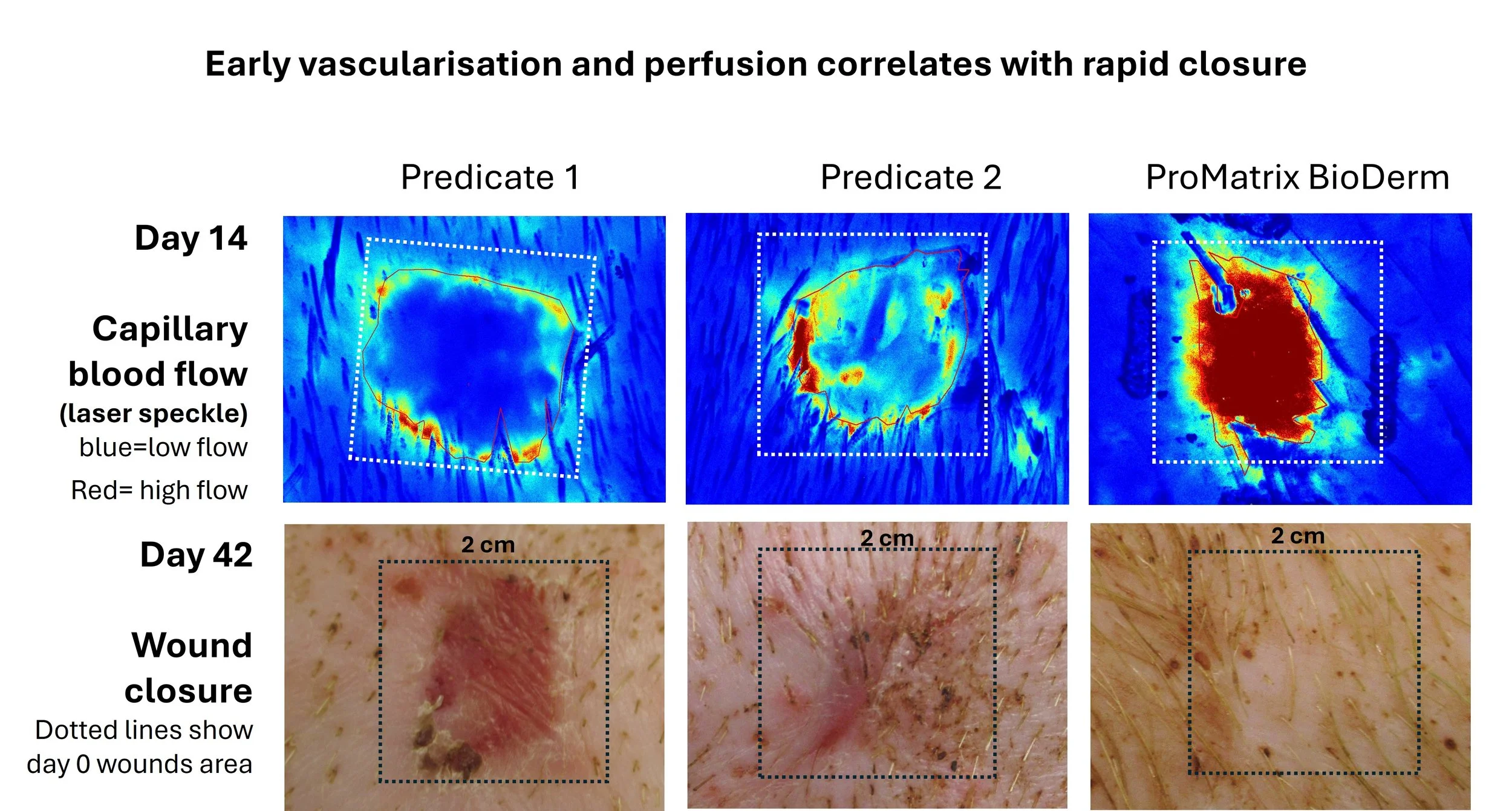
Skin excision wounds (2 X 2 cm square) grafted with with either two types of current commercial scaffold (predicates 1& 2) or ProMatrix BioDerm, on the day of excision. The extent of vascularisation into each scaffold at Day 14 and the visual outcome at Day 42 are shown.
ProMatrix - Changing the Paradigm of skin reconstruction
from ‘healing first, then treat the scar’
to
Preventing scar formation
Referencess:
Vaporidou et al, (2023) Adv Wound Care 12(10):574-600 (https://doi.org/10.1089/wound.2022.0050)
Zhou-G et al, 2023) Polymers. 15(5), 1151; https://doi.org/10.3390/polym15051151
Additional material
ProMatrix BioDerm pre-clinical evaluation
Summary of Oxartis’ Proof-of-Concept pre-clinical evaluation of ProMatrix BioDerm.